Implant Process
Suppose you've opted for dental implants as your preferred solution for replacing a missing tooth. Let's delve into the key steps that will unfold in this process.

Implant consultation

Implant planning with 3D X-ray


Implant consultation
1. Assesment
The initial phase of any dental implant procedure involves a comprehensive diagnosis and treatment planning process. Our skilled professionals conduct a meticulous evaluation of the patient's overall health, local health conditions, biomechanical and anatomical structures, as well as treatment certainties and uncertainties. Based on these assessments, our experienced doctors provide personalized recommendations to ensure the best course of action for each patient.
2. Additional Surgery (optional)
This option is specifically recommended for patients with insufficient bone at the implant site, a common challenge in dental implant procedures.
In the accompanying image, the sinus lift and bone augmentation/grafting procedures are illustrated. These advanced techniques involve creating additional bone volume to enhance the foundation for implant placement at the site of the missing tooth. This ensures a secure and stable environment for successful implant integration, particularly in cases where natural bone density is limited.
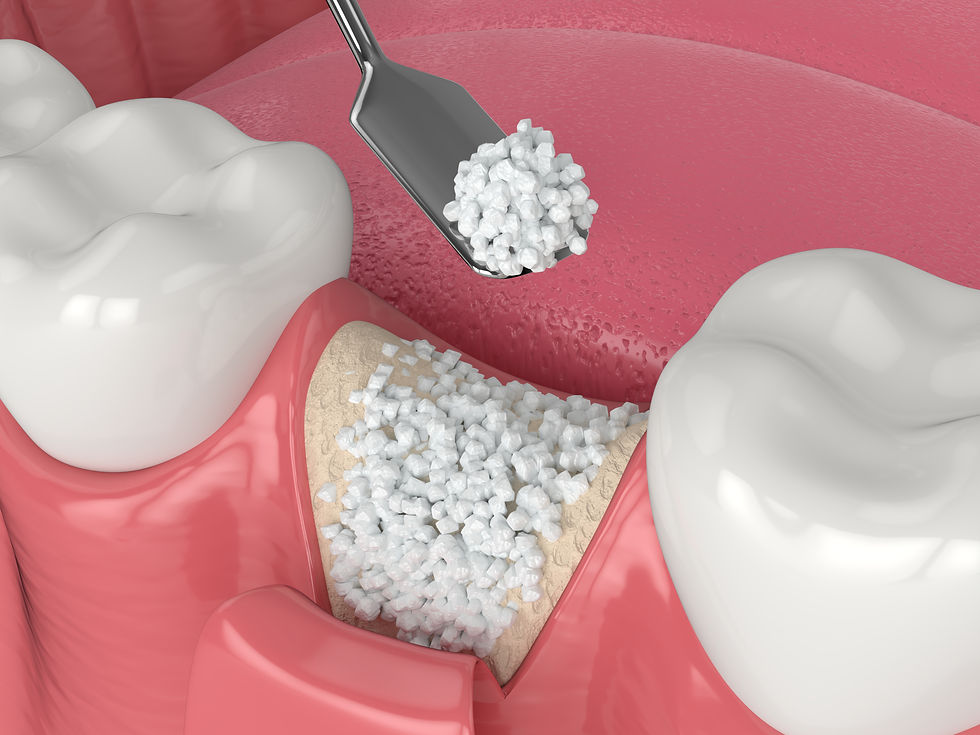
Bone grafting procedure

Bone grafting required implant site

Post sinus lift and bone grafting surgery

Bone grafting procedure




3. Implant Placement
Preceding the surgical procedure, the patient will be administered either a local anesthetic or general anesthesia, tailored to individual preferences and medical considerations. Subsequent to the anesthesia taking effect, the procedural phase commences. An incision is meticulously made, exposing the designated implant site. A sequence of progressively wider drills is employed to incrementally attain the requisite socket dimensions for optimal implant placement. The implant is subsequently securely positioned within the prepared socket.
Step 1 and 3 can happen on the same visit depending on quantity and quality of original bone.
4. Healing
Following the completion of the surgery, a crucial healing period ensues. Ensuring the full and biological integration of the fixture with the bone is paramount before progressing to the subsequent steps. Concurrently, the doctor will craft a provisional restoration (temporary restoration) to mitigate any social discomfort for the patient during this interim period with a missing tooth.

Before suture removal
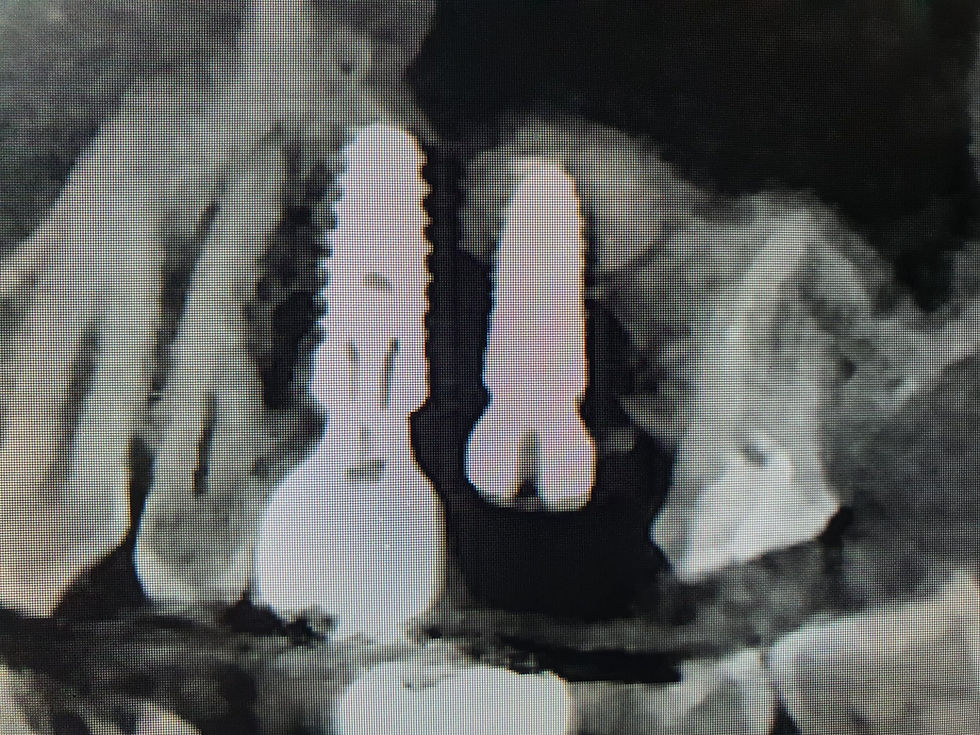
Post suture removal X-ray showing stable placement of implant.

Before suture removal



5. Final Restoration
Upon the full healing of the surgical site, the stage is set for the final restoration. An impression, capturing a detailed negative imprint of both hard and soft tissues, is meticulously crafted and dispatched to the dental lab. Leveraging the anatomical data derived from the impression, the dental lab proceeds to meticulously construct a personalized prosthesis. The concluding step involves affixing the final prosthesis into the patient's mouth, thus concluding the comprehensive dental implant treatment.
Treatment Details

3-6 Months
Duration
.png)
3-7 Visits
Required

Local Anesthetic
Required

Regular Visit
Regular Visits required for the maintenance
Frequently asked questions
Q1. Is Implant permanent? Dental implants are designed to be a long-term and durable solution for tooth replacement, and for many individuals, they can be considered permanent. The implant itself is a titanium post that is surgically placed into the jawbone, where it fuses with the bone through a process called osseointegration. This provides a stable foundation for a dental crown, bridge, or denture to be attached. The longevity of a dental implant depends on various factors, including: Maintenance, Health, Quality of Bone etc. While dental implants are intended to be a long-lasting and reliable tooth replacement option, their permanence is influenced by various factors, and individual experiences may vary. It's crucial to discuss expectations and maintenance with your dental professional to ensure the best possible outcome for your specific situation.
Q2. Do I need bonegrafting surgery? Whether or not you need bone grafting for implant surgery depends on the current condition of your jawbone. A sufficient amount of healthy bone is essential for the stability and success of dental implants. Here are some scenarios where bone grafting may be required: Insufficient Bone Volume: If there isn't enough bone in the implant site due to factors like tooth extraction, periodontal disease, or natural bone resorption, a bone graft may be necessary to augment the bone volume. Bone Density Issues: In some cases, the existing bone may lack the density required to support an implant. Bone grafting can enhance bone density, providing a stronger foundation for the implant. Sinus Augmentation: For implants in the upper jaw, near the sinus cavity, a sinus lift or augmentation may be necessary to create enough space for the implant and prevent interference with the sinus. Ridge Modification: If the jaw ridge is too thin or uneven, ridge modification through bone grafting can reshape the bone to better support the implant. Your dentist or oral surgeon will assess your oral health, review X-rays or CT scans, and determine whether bone grafting is needed based on factors such as the location of the implant, the quality and quantity of existing bone, and your overall health. If bone grafting is recommended, it is typically done before the implant surgery to allow time for the grafted bone to integrate and provide a stable foundation for the implant. It's essential to have a thorough consultation with your dental professional to discuss your specific case and understand whether bone grafting is necessary for your dental implant surgery.
Q3. How long does it take to have the implant tooth? The treatment duration for implants varies based on bone strength. For strong bone, it's typically 3 to 4 months, while for cases with insufficient or weak bone, it may range from 6 months to 1 year.
Q4. I have high blood pressure and diabetes. can I do implant surgery? Having high blood pressure and diabetes doesn't necessarily disqualify you from getting dental implant surgery, but it does require careful consideration and coordination with the doctor. Both conditions can impact the healing process, so it's crucial to manage them effectively before undergoing implant surgery.

